Biochemical Foundations of Human Nutrition
Andrea Bellelli
Dipartimento di Scienze Biochimiche "A. Rossi Fanelli"
Sapienza Universita' di Roma
1. CALORIES FIRST!
The metabolic requirements of humans range between 1,500 and 4,500 kcal/die or more.
This amount must be supplied by the diet and accounts for energy production (heat, muscular work, cardiac work, etc.) and tissue turnover.
Every diet in every climate satisfies these requirements, except during major catastrophes (e.g. famine, civil war, deportation and refugees, etc.). Malnutrition is the clinical condition associated to chronic insufficiency of dietary intake.
2. CALORIES IN RELATION TO ORGAN REQUIREMENTS
Calories are mainly provided by sugars, fats and proteins; only to a very small extent by nucleic acids contained in the diet.
The human brain amounts to 2% of the body mass and uses up to 20% of the calories provided by the diet. Its (almost) only nutrient is glucose. Its daily energy requirement amounts to 240 kcal/kg.
The liver and kidneys use mixtures of all nutrients and their daily energy requirements are 200 and 440 kcal/kg, respectively.
Skeletal muscles and the heart derive some 70% of their energy from the metabolism of saturated fatty acids; their daily energy requirements under rest conditions are 13 and 440 kcal/kg, respectively.
References
Wang Z. et al. (2010) Specific metabolic rates of major organs and tissues across adulthood: evaluation by mechanistic model of resting energy expenditure. Am J Clin Nutr. 92: 1369-77.
Belanger M. et al. (2011) Brain Energy Metabolism: Focus on Astrocyte-Neuron Metabolic Cooperation. Cell Metabolism, 14, 724-738
3. COMPOSITION OF THE DIET IN RELATION TO ORGAN REQUIREMENTS
Given the specific requirements of nutrients of the different organs one may roughly indicate that the diet of a healthy adult should include no less than approximately 700 kcal/die in sugars, 300 kcal/die in proteins and 300 kcal/die in fatty acids; above these values and up to the total energy intake the composition is free and left to the preferences of the individual (or at least this is the view point of a biochemist).
This estimate is drawn from the sum of the resting, organ-specific dauly requirements and neglects the possible interconversions of sugars and aminoacids. It will be remarked that the amount of necessary fats is low, and amounts to some 30-35 g of any vegetable oil. This is because every nutrient, if in excess, is converted to fatty acids. The requirement is calculated on the average content of essential nutrients of lipophilic nature, e.g. essential unsaturated fatty acids (see below).
It is important to consider also some drawbacks of some nutrients. Fatty acids, if of animal origins, are usually associated to cholesterol, and a fat rich diet may cause increased levels of cholesterol of alimentary origin. Aminoacids must be de-aminated before being used for energy production; the ammonia thus released is converted to urea via the urea cycle and excreted by the kidney. Excess aminoacids in the diet cause a nitrogen overload and an increased work of the kidney, which may not be well tolerated in the elderly or in patients suffering of kidney disease.
4. ESSENTIAL NUTRIENTS
The diet should not only satisfy the specific energy requirements of all the organs of the organism, but should also provide a sufficient amount of the essential nutrients, substances that the organism requires but cannot syntehsize by itself: vitamins, essential aminoacids, polyunsaturated fatty acids and some other compounds.
Polyunsaturated fatty acids are not synthesized by our metabolism: we only synthesize saturated and monounsaturated (monoenoic) fatty acids. These compounds are required for several reasons, the most important of which is the biosynthesis of prostaglandins, leukotrienes and tromboxanes.
Vitamins cannot be synthesized by our metabolism and play a host of vital roles, mostly as coenzymes. They may be water-soluble or lipid-soluble. Lipid-soluble vitamins, together with essential fatty acids are the main reason why our diet cannot be fat-free even though we can synthesize the fatty acids required by the heart and skeletal muscles.
Essential aminoacids are required for protein turnover. Proteins of animal origin are richer in essential aminoacids than those of vegetable origin.
5. THE QUALITY OF THE DIET
A "good quality" diet satisfies the daily requirements of the whole organism without requiring excess caloric intake; a "low quality" diet is one whose composition either does not satisfy the specific requirements or requires excess caloric intake to do so (this is the reason why under some circumstances a patient may both be obese and suffer of some specific dietary deficiency).
Some diets may be low quality but still perfectly compatible with life and health if the energy requirements are high (e.g. the diet of the Inuit people in the Arctic, which amounts to over 4.000 kcal/die: its composition, by weight, is very unusual since foods of vegetable origin are almost absent, and the diet is very low in sugars; but it is very high in animal proteins and fats from marine mammals, rich in unsaturated fatty acids).
6. ESSENTIAL CATABOLIC (ENERGY PRODUCING) BIOCHEMICAL PATHWAYS: THE KREBS CYCLE, BETA OXIDATION OF FATTY ACIDS, GLYCOLYSIS AND THE UREA CYCLE
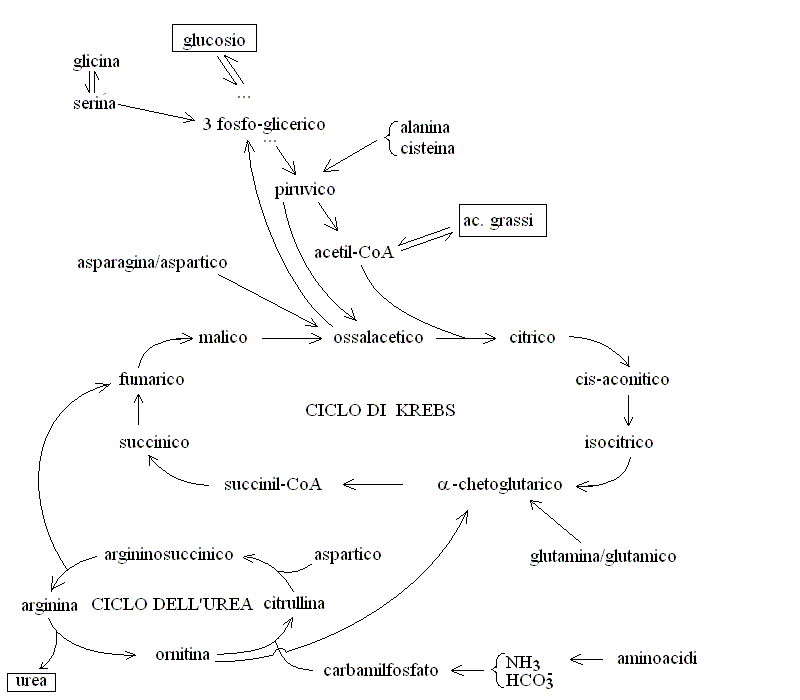
7. CATABOLISM OF AMINO ACIDS
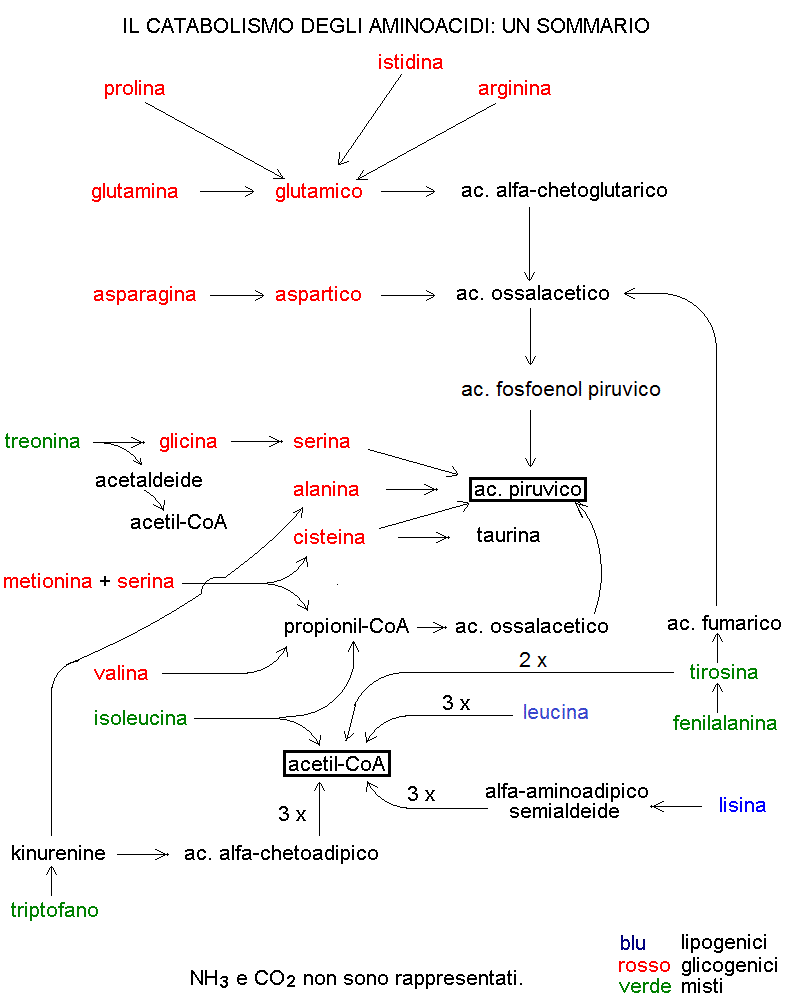
8. METABOLISM DEAD ENDS AND INTERCONVERSION OF NUTRIENTS
The basic form of energy reserve in animals is triglycerids in the fat tissue: if too much calories are provided by the diet these are converted to fatty acids and stored in adipose tissue; obesity may ensue.
A paradoxical problem of obesity is that fatty acids can only be used as energy sources (or, at most for the biosynthesis of cholesterol and its derivatives), and thus cannot provide nourishment for the brain and many other tissues: some amount of dietary sugar is necessary even though one may want to consume fat reserves. Animals cannot convert fatty acids into sugars or aminoacids.
Aminoacids of the glycogenic type can be used to produce glucose (by gluconeogenesis) and glucose metabolites can be used to produce non-essential aminoacids, provided that a source of ammonia is available. If the dietary intake of sugars is low aminoacids are converted into glucose to feed the brain; if both aminoacids and sugars are low, proteins from the muscular tissue are degraded and converted to glucose. Thus, fasting is not a convenient way of consuming the body fat, as it leads to muscular wastage.
The fundamental possibilities to intervert nutrients are reported in the picture below: sugars and aminoacids can be converted to lipids (via acetyl-CoA) but the reverse concersions are impossible; glycogenic aminoacids can be converted to glucose; and glucose can be converted to glycogenic aminoacids if enough ammonia is available:
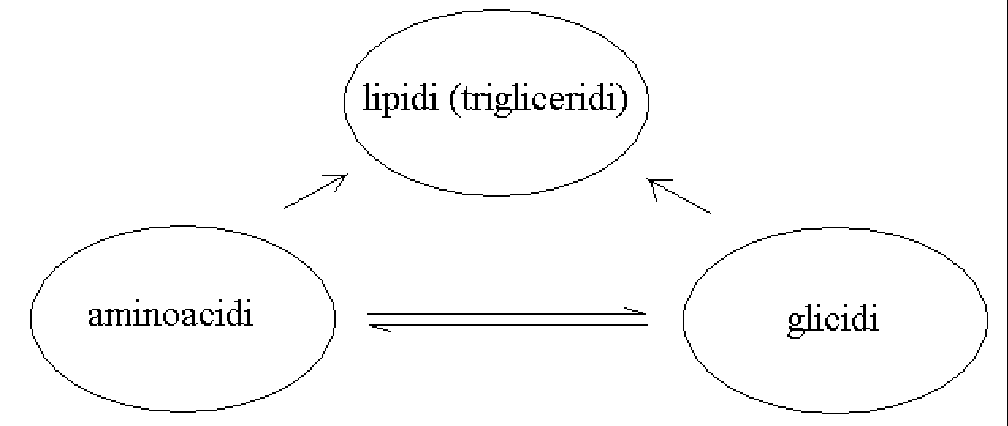
As a consequence of the above described possible interconversions of nutrients one may partially correct the estimates of the diet composition: i.e. where we write down "700 kcal/die in sugars, 300 kcal/die in proteins and 300 kcal/die in fatty acids" we know that partial replacement of sugars with proteins/aminoacids is possible; fatty acids, however, cannot replace either. Moreover, replacing sugars with aminoacids, implies a substantial change in nitrogen metabolism with increased production of urea and increased renal work: possible does not mean advisable.
9. REGULATION OF FOOD UPTAKE; HUNGER
We are aware of the complex caloric requirements of our body, because of the sensation of hunger, which is largely controlled by hormones. UNfortunately we are not aware of the requirements of essential nutrients: only caloric deprivation is associated to a sensation. Thus we can recognize a low-calories diet (because we are hungry) but not a low-quality diet, lacking vitamins or other essential components.
Leptin, or the satiety-hormone
The regulation of food uptake is complex. The main pathway involves the hypothalamus which releases a family of hormone-like substances, called the Y-neuropeptides, that stimulates the sensation of hunger and promote food intake. Release of the Y-neuropeptides is inhibited by leptin, a protein hormone released by the adipose tissue. The system leptin + Y-neuropeptides uses a negative feedback: the more abundant the fat tissue, the more leptin is produced and the less Y-neuropeptides are released. Thus the adipose tissue effectively reduces the sensation of hunger. Unfortunately the system is subjected to adaptation and the negative feedback loop looses effectivity under prolonged excess caloric intake.
Ghrelin, the hunger-hormone
Another hormone-like peptide capable of stimulating the sensation of hunger in the brain is ghrelin, produced by the empty stomach (and to a lesser extent by the pancreas). Dilatation of the stomach causes blockade of the release of ghrelin.
Grelin antagonizes insulin release and excess ghrelin causes an increased glycemic peak after meals; it has been implicated in (some cases of) type II diabetes, associated to obesity. On the contrary, the normal response to feeding is ghrelin decrease and increased secretion of insulin, that quenches the post-prandial hyperglicemia.
10. IS OBESITY A DESIRABLE CONDITION?
Obesity is associated to a host of health problems, thus one should expect to be counter-selected by evolution. The widespread diffusion of this condition strongly suggests the contrary: obesity is in some way a desirable condition.
The reason, of course, is that during the evolution of mammals conditions of famine were common. The sensation of hunger is therefore regulated to promote excess food intake whenever food is available, to protect the animal from starvation in conditions where food is scarce. Nowadays obesity is common because famines are rare.
The "thrifty" (frugal) genotype, associated to a genetically determined type II diabetes was studied by the geneticist James V. Neel, in 1962. He proposed that the diffusion of this disease in some ethnic groups was due to a selective advantage since the affected individuals would fatten faster than normal individuals and would thus be better protected during famines.
Genetic mutations of leptin or the leptin-receptor cause obesity in humans, as does overproduction of ghrelin.
References
Clement K. et al. (1998) A mutation in the human leptin receptor gene causes obesity and pituitary dysfunction. Nature. 392: 398-401
Neel J.V. (1962) Diabetes mellitus: a "thrifty" genotype rendered detrimental by "progress"? Am. J. Hum. Genet. 14: 353-362.